WASHINGTON — Ever since the coronavirus pandemic started to sweep across America, U.S. Air Force Staff Sgt. Max Estrada’s daily routine has been the same. He wakes up, logs onto his computer for a virtual meeting with his team and then heads to his garage for a marathon session of 3D printing.
Estrada is the noncommissioned officer in charge of agile manufacturing at Phoenix Spark Lab, which is made up of small cell of airmen at Travis Air Force Base, California. They use emerging technologies to try to find innovative solutions to problems at the installation. Normally, the lab’s activities include inventing widgets for military aircraft, but over the past couple of weeks its focus has been generating medical equipment, specifically 3D-printed face shields and face masks.
“I sit there for about a good 12 hours a day of my time, just trying to get this done and get people what they need,” Estrada told Defense News. “There’s a coffeepot, a little Bluetooth speaker, my computer and the sound of printers all day.”
RELATED
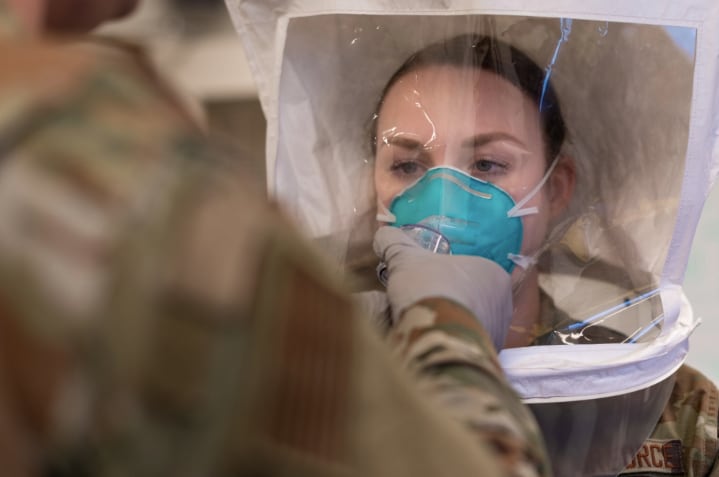
So far, 20 face shields have been delivered to Travis AFB’s medical community for testing, with another 20 slated for delivery this week. The eventual home for this medical equipment is the base’s David Grant USAF Medical Center, the Air Force’s largest medical facility, which will use them to extend the life of N95 masks that are in short supply across the globe.
Estrada is one of three members of the lab who are working from home, printing plastic headbands that form a face shield when combined with clear, plastic sheeting. The cadre has four 3D printers in operation, and each printer can make headbands for two shields over a 2-hour period, said Senior Master Sgt. Phillip Edwards, the 60th Air Mobility Wing Phoenix Spark superintendent.
“We’re looking at an output of about 15 to 20 a day. We can expand that output using other folks that we have in our network, and we could probably get up to 30 a day,” Edwards said. “We’ve got a couple [additional printers] in the lab, but for obvious reasons we’re trying to avoid being in the lab and on base.” Edwards was likely referring to the practice of social distancing, which medical experts have recommended as a course of action to prevent the further spread of COVID-19.
The face shields are based on a template made by Czech 3D-printing hobbyist Josef Prusa, with a design that Estrada then modified to allow for a more secure fit and so that the plastic sheeting over the face can be removed and decontaminated.
Estrada had originally intended to make 3D-printed N95 masks, but those items would need additional testing and approval to ensure they meet the same filtration standards as N95 respirators approved by the U.S. Food and Drug Administration, he said. Instead, the lab pressed forward with making shields and mask covers that be worn over other medical gear, then disinfected and reused.
RELATED

While making face shields doesn’t directly ameliorate the scarcity of N95 masks, it ensures that the medical organizations at Travis don’t exacerbate that shortage by contributing to demand, said Lt. Col. Aaron Weaver, the flight commander of the 60th Bioenvironmental Engineer Squadron.
“If you think about a face shield, it covers the entire face,” he said. “It protects that mask, and it extends the use of it.”
But there have been challenges in ramping up production of the face shields. At first, the lab found that it couldn’t cut out the clear, plastic face coverings quickly enough to match the pace at which headbands were made with the 3D printers. Edwards said the lab had initially cut by hand each face shield individually with a knife until just recently, when it partnered with the 60th Maintenance Squadron, which has a laser cutter that it can use to make shields more quickly.
“That will keep up with production of about 30 head straps a day, and then we’ve got more capacity — more bandwidth — with other folks’ printers in the community we have here,” he said.

Still, other obstacles remain. All of the printers used by the lab make an object by heating up plastic filament and extruding it into a specific shape, Estrada said. But the different polymers needed to make the headbands aren’t widely available at major retailers like Walmart or Home Depot, and they must be ordered online and delivered.
“Getting that material to us can be a challenge, especially with how much we’re having to print, both in the iterative process of trying to redesign something that’s exactly what the medical group wants, in addition to having to mass produce to the standard that we need,” he said. “I think that’s been an issue.”
Travis AFB isn’t the only military base trying to use its 3D-printing equipment to create protective gear for medical workers. Similar manufacturing efforts for face masks and shields are taking place at Goodfellow AFB in Texas, Nellis AFB in Nevada, Eielson AFB in Alaska and Dover AFB in Delaware, among other locations.
Nine Navy and Marine Corps commands have also begun 3D printing face shields to support a Federal Emergency Management Agency request, according to an April 2 news release.
Valerie Insinna is Defense News' air warfare reporter. She previously worked the Navy/congressional beats for Defense Daily, which followed almost three years as a staff writer for National Defense Magazine. Prior to that, she worked as an editorial assistant for the Tokyo Shimbun’s Washington bureau.








